After surgery, your child will need some time to recover. There may be some changes or complications from the surgery. As a parent or caregiver, you can help your child with rehabilitation and providing care at home.
What happens after the surgery?
Your child may first go to a post-anaesthetic care unit (PACU) for several hours after the surgery. Generally, your child may be brought to a critical care unit (CCU), intensive care unit (ICU), where they will be watched overnight. You are welcome to visit your child here, but sometimes the nurses may be busy caring for your child and you may have to wait to see them. Some children may need help with a breathing machine (ventilator) for a few days. The doctors will decide when they are well enough to go to the neurosurgical ward. In some cases, your child may go directly to the neurosurgical ward from the PACU.
When you see them for the first time after the operation, they will look different than they did before. They may have a small bandage or a big white bandage, like a turban, on their head. This bandage will be removed in two to three days.
Their face may be swollen or bruised. Their eyes may be puffy or swollen shut. This is all expected. It may get worse up to three days later, and then get better. The dexamethasone your child is receiving to reduce swelling around the tumour does not prevent swelling of the face and eyes.
Your child will be attached to monitors and different tubes. The machines may be noisy. This does not mean there is a problem. These machines help the treatment team see how well your child’s body is handling the operation. Here are some of the machines they may be attached to:
- An intravenous (IV) line will make sure he has enough fluids. This line also delivers medicines such as antibiotics and pain medicines.
- Various monitors will keep track of their heart rate and oxygen saturation.
- An arterial line will check blood pressure and can be used to take blood samples.
- A tube called a urinary catheter may be inserted into the bladder to drain their pee (urine). The catheter is usually taken out after one day.
- The normal flow of cerebrospinal fluid (CSF) in your child’s brain may be disturbed because of swelling after the operation. Your child may have a temporary tube called an external ventricular drain (EVD) to drain fluid from the ventricles in their brain to a bag outside the body. This helps while the brain recovers from surgery.
You can ask your child’s nurse if you have any questions about any of these machines and tubes.
Within the first days after the surgery, your child will have an imaging scan (MRI or CT) to see how much tumour has been removed, and that everything is all right.
How will my child feel after the surgery?
Your child may notice some changes after the operation. Many of these will not last long. They will continue taking pain medicine and steroids (dexamethasone). In addition, here are some of the changes your child might talk about, or you might see:
- Tiredness
- Headaches
- Pain around the surgical incision (cut). If you can sense that your child is in any pain, you need to let the treatment team know. They will be given some medicines to feel better.
- Constipation: The pain medications or lack of activity may cause constipation. This can be managed with medicine.
- Nausea or vomiting: They may be given medicine for this.
- Problems talking: For instance, their words may slur together. They may be given some exercises to make the muscles in their tongue and jaw stronger.
- Problems eating or drinking because they can’t swallow. There are certain symptoms you can watch for. The treatment team will help with this problem.
- Physical problems, such as clumsiness (ataxia), weakness on one side of the body, or poor balance.
- There may be a small bulge in the skin near the incision. This is a small pool of cerebrospinal fluid (CSF). The treatment team will check this. It should go away in a few weeks. It is called pseudomeningocele.
- Some children may be given medicine to prevent seizures. If your child has a seizure, they will be given more medicine to stop the seizure.
- If your child had a tumour in the back of the head (posterior fossa), they may have a condition called transient mutism. This means they may not be able to speak after the operation for some time.
What can I do to help my child get better after surgery?
Within a day or two after the operation, a new team of experts will be working with your child to help them recover from the operation. This team could include a physical/occupational therapist, a dietitian, a child life worker, and a speech-language pathologist. Talk to these team members about what you can do. For example, your child will begin to sit at the edge of the bed, and progress to sitting in a chair one or two days after surgery. Your nurse or physiotherapist will help you and your child with this activity. You can also help to participate in their daily care, such as bathing and dressing.
Creating a friendly and healing environment will help as well. Make sure your child has familiar items from home, such as family photos or favourite toys. Limit the number of visitors so that your child — and you — don’t get too tired.
This is also a good time to take care of yourself and get some rest.
What to watch for after the surgery
Problems, or complications, after brain tumour surgery are not common. To be safe, you should watch for certain symptoms in your child after the operation, and when you go home. These symptoms might mean that your child has a complication. Contact their treatment team right away if you notice any of these symptoms.
- fever (a temperature of 37.8°C / 100.0°F taken under the arm, or 38.5°C / 101.3°F taken in the mouth)
- redness or swelling along the surgical incision
- fluid coming from the incision
- headaches
- vomiting
- any other concerns you have
What is a complication?
A complication is a medical problem that occurs after surgery, treatment, or illness.
Rehabilitation after surgery
Your child may benefit from doing exercise therapy to improve any physical problems he may have. In the hospital, physical and occupational therapists will help your child and may show you some exercises. Once your child is at home, they may need to continue using the services of a physical-occupational therapist in the community.
There are some exercises you can do together with your child.
- After surgery, neck exercises will help your child get back neck movement.
- If your child is having balance problems, there are many balance exercises that can be done at home after your child leaves the hospital.
Neck exercises after neurosurgery
After neurosurgery, your child’s neck muscles may be sore and they may not be able to move their neck very far. Your child’s physiotherapist will choose which exercises are the most appropriate after surgery. By the time your child leaves the hospital, they should be able to perform each exercise.
A few points to remember:
- Your child should do all the movements by themselves — do not stretch your child’s neck.
- Your child should do these exercises while sitting down, with their arms resting comfortably on their lap.
- Each exercise should be done until your child feels a mild discomfort from the stretch.
- You may have to sit in front of your child and place your hands on their shoulders to prevent their shoulders from moving. This ensures that the movement comes from your child’s neck.
Neck Exercises
Do each exercise three times. Repeat all exercises three times a day.
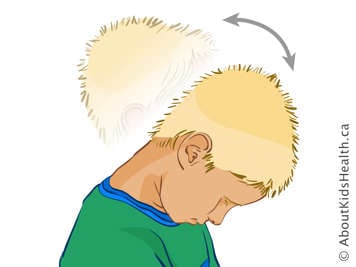
Neck flexion. Your child should bring their chin to their chest. Hold for 10 seconds and straighten up.
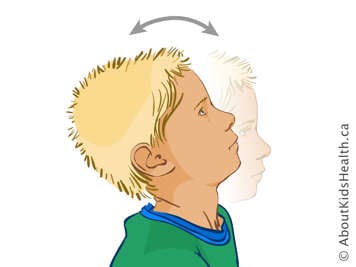
Neck extension. Your child should look up to the ceiling. Hold for 10 seconds and straighten up.
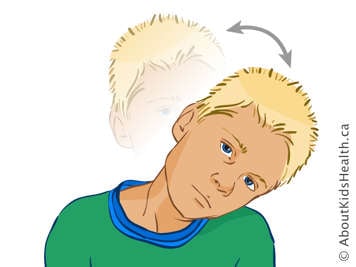
Neck side flexion. Your child should bring their ear to their shoulder on the right side. Hold for 10 seconds and bring the head back upright. Do three to the right side and then three to the left side. Make sure your child doesn’t lift their shoulder up to touch their ear.
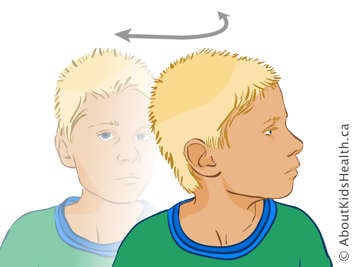
Neck rotation. Your child should turn their chin to their shoulder on the right side. Hold for 10 seconds and return to face forward. Do three to the right side and then three to the left side.
Balance exercises after neurosurgery
Your child may have balance problems caused by the tumour, the surgery, or both. You can help your child to do some exercises to improve their balance when they go home from the hospital. Check with your child’s physiotherapist before doing these.
A few points to remember:
- make sure that an adult is always present
- do these activities a few times a day
- pick two or three activities to work on at a time
- these exercises are generally suitable for children aged five and up
Balance Exercises

Practise walking on a curb with one foot in front of the other. Or put a piece of masking tape on the ground/floor and practice walking with one foot in front of the other. When this is easy, try this with the eyes closed.

Practise standing on one leg. Count how long your child can hold this position. Try to beat this record each time.

Once your child can balance on one leg easily, stand on the right leg and practise bending the right knee five times. Repeat with the left leg.
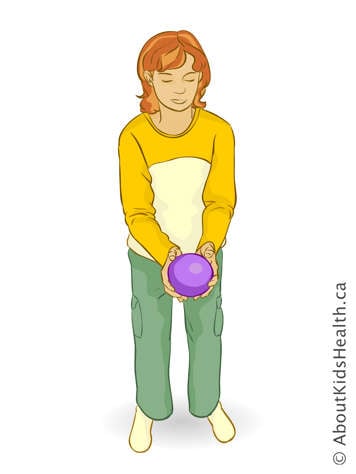
Play catch with your child. Once they can do this, make it more challenging by throwing the ball to the right or left side, up high or down low.

Practise kicking a ball with your child. Make it more challenging by kicking the ball to your right or left side so that they have to step and reach for the ball.

Practise walking backwards or sideways.
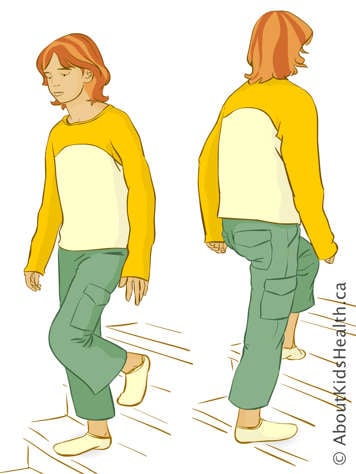
Practise walking upstairs or downstairs without holding onto a railing.

Practise walking on the toes and on the heels.
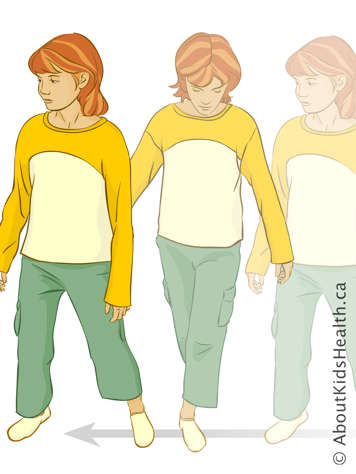
Practise grapevine walking — crossing over the feet.

Practise playing "Simon says" with your child. Use different movements to make it harder as it gets too easy.

Practise hitting a balloon back and forth with your child. Make sure there is lots of open space to avoid tripping.

Practise drawing numbers or letters in the air with the arms or legs.

Practise stepping up onto a step and back down again. When this becomes too easy, practise stepping over a small object and then back over it again.
When can my child go home after surgery?
Your child will not be sent home until they are medically stable. This may happen seven to 10 days after the surgery. However, this depends on the child and the type of operation they had. They must have no external drains, and be able to walk, eat, and drink on their own, or have a plan in place to be sure these needs are met. Before they come home, the treatment team will have a plan in place to help your child get better. This is called a rehabilitation plan. A discharge planner may work with you to organize the details. Your child may need home care, such as a physical/occupational therapist. In some cases, if they need extra care, they may be sent to a rehabilitation hospital.
If your child needs additional treatment, such as chemotherapy or radiation, the treatment team will meet you and provide information about dates and times for appointments. Ask them if you are not sure. This treatment will begin soon after they are discharged.
You will have to bring your child for regular follow-up appointments. The first surgical appointment after the operation is usually six to eight weeks after they are discharged. The surgeon will check the incision and the shunt at this time.
If you have any questions, contact the neurosurgical ward.
Before you go home
A discharge planner will know what your child needs and will help you plan for your child’s return. Your child’s treatment team will also explain how to take care of your child when they come home. Some of the areas they may talk about are:
Caring for the incision (surgical cut)
- Keep the incision clean.
- Do not touch it or pick it.
- Do not put direct pressure on the incision.
- Do not put your child’s head underwater in a bath or pool for at least 10 days.
- Your child can wash their hair with any type of shampoo three days after the operation.
- Depending on the type of stitches, they will either dissolve or need to be removed by your child’s family doctor or paediatrician. The team will let you know what to do.
Getting home from the hospital
You need to think about how you will get your child home from the hospital. Please consider these questions:
- Will your child be able to get in and out of your family car?
- Can you buckle your child safely into a seat belt or booster seat? If your child is an infant, will they fit into a car seat?
- Are you planning to take your child home from the hospital by bus, train or airplane? If so, please contact your discharge planner before booking your ticket. They can help you make special arrangements with the transportation company.
Caring for your child at home
Caring for your child when they get home from hospital will take a lot of time and energy. If you have other children at home you may need extra help. Think about the following questions:
- Who will be caring for your child when they come home?
- Will you or a helper be able to lift or carry your child from the bed to a chair or the toilet if needed?
- Do you have family or friends who will be able to help you if needed? You may need help with things like grocery shopping, cleaning, and laundry.
