What is spina bifida?
The spinal cord is a thick bundle of nerves that carries messages between the brain and the rest of the body. It floats in a liquid called cerebrospinal fluid (CSF). This liquid nourishes and protects the brain and spinal cord. The CSF is covered by a lining made of three thin layers called the meninges. This lining is normally protected by the bones of the spine (the vertebrae).
In people with spina bifida, the bones that protect the spinal cord have not formed completely while the baby is developing in the mother's womb. This leaves the lining, the CSF and the spinal cord unprotected. This happens very early in pregnancy.
Spina bifida can happen anywhere along a baby's back between the neck and the hips. It happens most often in the lower back. This area is called the lumbar or lumbosacral spine.
Children with spina bifida may have health problems because of this condition. They may experience changes or loss of feeling in their legs, have decreased movement of their legs or not be able to move their legs at all. They may also have problems with their bladder and bowel function, and have learning challenges.
About 2.6 in every 10,000 babies are born with some form of spina bifida.
The four main types of spina bifida
There are four main types of spina bifida:
- spina bifida occulta
- lipomyelomeningocele
- meningocele
- myelomeningocele
"Meningo" refers to the lining of the vertebral canal. "Myelo" refers to the spinal cord itself. "Cele" means a sac or something bulging out.
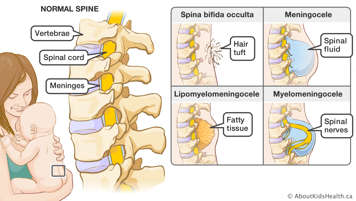
Spina bifida occulta
Spina bifida occulta is the mildest form of spina bifida. It occurs when a small section of the outer part of one or more of the vertebrae (the bones of the spine) has not completely closed, leaving an opening. In this type of spina bifida, the spinal cord and its coverings (the meninges) are usually not damaged and they do not protrude or bulge through the opening. There may be a dimple, tuft of hair, birthmark or fatty bulge at the site of the defect. This type of spina bifida may not be detected before birth. Many people may have this type of spina bifida and not be aware of it.
Lipomyelomeningocele
A lipomyelomeningocele is a form of spina bifida where the outer part of one or more of the vertebrae has not completely closed, leaving an opening. Some abnormal fatty tissue pushes through the opening and may cause compression of the nerves or abnormal formation of the spinal cord.
Meningocele
A meningocele is a more severe form of spina bifida. It occurs when the outer part of the vertebrae has not completely closed, leaving an opening. The meninges (covering) are pushed through the opening to form a sac. The spinal cord is not pushed into the sac, so the nerves may not be as severely affected. This sac is often covered with skin.
Children with a meningocele may have normal movement and normal feeling in their legs and feet.
Myelomeningocele
A myelomeningocele is the most severe form of spina bifida. It occurs when the outer part of the vertebrae has not completely closed, leaving an opening. With a myelomeningocele, both the covering of the spinal cord (the meninges) and the spinal cord itself are pushed out through the opening. Usually they protrude into a covered, fluid-filled sac that has a very thin membrane (not covered by skin). Because part of the spinal cord bulges into the sac, the spinal cord fails to develop properly and nerves are damaged. Most children with a myelomeningocele will have difficulty with movement and feeling in their legs and feet.
Causes of spina bifida
All the causes of spina bifida are not known but there are genetic, environmental and nutritional risks linked to spina bifida. It is important to note that no one factor alone is thought to be responsible. A combination of factors, possibly among other unknown factors, may contribute to the development of spina bifida.
- Some spina bifida is found in families, meaning there may be a genetic link.
- What a pregnant individual eats months before pregnancy and during the first 28 days of pregnancy may influence risk.
- Some medications that interfere with the body’s ability to use folate and folic acid could increase the risk of spina bifida.
- Pregnant individuals with diabetes whose blood sugar is not well controlled have a higher risk of having a baby with spina bifida.
Spina bifida and other neural tube defects are less likely to occur when pregnant individuals get enough folic acid in the months before and during early pregnancy. If there is any possibility of becoming pregnant, it is important to have a well-balanced diet rich in folic acid. If an individual is planning to become pregnant, it is essential they begin taking folic acid daily, at least three or four months before trying to conceive. The usual recommended dose is 400 micrograms (mcg) of folic acid a day. Often this can be found in a prenatal vitamin. If an individual has had a pregnancy affected by spina bifida, or a family history of spina bifida or is taking certain medications, they may require a higher dose of folic acid.
Diagnosis of spina bifida
Spina bifida can be diagnosed during pregnancy or after the baby is born.
During pregnancy
There are tests that can be done during pregnancy that can indicate if the fetus has a high chance of having spina bifida.
- Alpha-fetoprotein (AFP) blood test – AFP is a protein made by the fetus. AFP crosses from the fetus through the placenta to the mother. A test is done that measures AFP levels in the pregnant individual's blood. If there are high levels of AFP, this might mean the fetus has spina bifida.
- Ultrasound – this is a common test during pregnancy that allows health-care providers to see images of the fetus. In some cases, an ultrasound can show if the fetus has spina bifida.
- Amniocentesis – this is a test that takes a small sample of the amniotic fluid that surrounds the fetus. If this fluid has a higher than average level of AFP then the fetus might have spina bifida.
- Fetal MRI – if initial tests suggest there is a high chance of spina bifida then a fetal MRI can be done. This is an MRI that is done on the pregnant individual to assess the fetus.
Spina bifida occulta may not be diagnosed until after birth, late childhood, adulthood or may not be diagnosed at all.
Treatment of spina bifida
Meningocele and myelomeningocele are both treated with surgery. In some cases this surgery may be done before a fetus is born (prenatal surgery). There are specific criteria for prenatal surgery that are determined by a specialized obstetrics team. This can be discussed with the obstetrics and NICU teams. In other cases, surgery is done shortly after birth. Older infants and young children with lipomyelomeningocele may require surgery if they develop symptoms. Spina bifida occulta does not usually require treatment.
To learn more about the treatment of spina bifida please read Spina bifida: Treatment and caring for your child after surgical repair.
Health problems linked to or caused by spina bifida
Every child with spina bifida is different with their own medical, mobility and learning needs. Some children may only be mildly affected while others may have more significant disabilities. Being born with spina bifida can bring life-long challenges. Your child’s health-care team will work together with you to help your child achieve their greatest potential.
The following health issues are common for children with spina bifida.
Hydrocephalus
Over 80 percent of babies born with spina bifida, primarily those with myelomeningocele, will also have hydrocephalus. Hydrocephalus is an abnormal build-up of CSF in the ventricles inside the brain, causing enlargement of the ventricles. Surgery may be required to treat the build-up of CSF.
Chiari malformation
Nearly all babies born with myelomeningocele have a Chiari malformation type 2. This is when the lower part of the brain (the brainstem) sits too low in your child’s upper spine area. Some children with Chiari malformation type 2 may have feeding problems (for example, weak suck when feeding, gagging, choking, trouble swallowing), sleep apnea or weakness of the arms. Surgery may be required to decrease the pressure on the lower part of the brain.
Leg function (movement) and sensation (feeling)
In children with spina bifida, the nerves in the spinal canal are often damaged or improperly formed. This can affect both feeling and movement in the legs. Some children may not be able to feel or move their legs at all, while others can stand and walk (with or without the help of equipment).
Muscles and bones
Muscles and bones may also be affected by spina bifida. For children with spina bifida, damaged nerves may mean they are unable to control their muscles properly. The position of the lesion on the back determines which muscles in the trunk and legs work. Generally, the lower the lesion is on the back, the more likely the muscles in the legs will work.
A baby with spina bifida may be born with clubfoot, this is when the baby's feet are turned in at the ankle.
The baby's hips may also be affected as different muscles may be stronger than others interfering with how the hips move and function. This can cause dislocation of the hip.
Muscles around the spine may also be affected. Any difference in muscle strength can affect the position of the spine and cause an abnormal curve called scoliosis. Children with spina bifida who have muscle and bone issues may need bracing or orthopaedic surgery.
Bladder problems
With spina bifida, the nerves that tell the bladder it is full, and to empty and release urine (pee) are often weak or not working. This means that babies and children with spina bifida may need help to pee and empty their bladder. When your baby is born, a catheter will be put inside their bladder through the urethra every few hours to see if they can pee on their own and empty their bladder. The urethra is the tube inside the body that carries urine from the bladder to the outside of the body. If your baby is unable to fully empty their bladder, they are at risk for urinary tract infections or possibly kidney issues. You may need to learn how to empty your baby’s bladder using a catheter before you can take them home. As children with spina bifida grow, they may also need further bladder testing, medications to help with urinary leaking, or surgery to help control their bladder and their ability to use a catheter by themselves. A member of the urology team will talk to you about this.
Bowel problems
Bowel function is controlled by nerves that are located in the bottom section of the spinal cord. Because of this, many children with spina bifida have differences in bowel function. Constipation is seen in almost all children with spina bifida. If bowel movements cannot be regulated with diet, fluids and toileting routines, other strategies including medications, suppositories, enemas or surgery may be needed.
Latex allergies/sensitivity
Babies with spina bifida have an increased chance of developing a latex sensitivity or allergy. It is important to make sure that products such as gloves, catheters and soothers do not contain latex.
Tethered cord
The spinal cord is normally elastic. In children with spina bifida, the spinal cord can get stuck at the site of the lesion and this is called a tethered cord. It is often stretched over time. That stretch can lead to injury of the spinal cord. Surgery may be required to treat tethered cord if it is causing symptoms.
Learning
Many children with spina bifida have difficulties in specific areas of learning. Your child may or may not have difficulty with some types of learning (such as attention and impulse control, memory, problem solving and visual spatial skills). Special testing by a psychologist may be needed to assess learning challenges. Some children may require educational support strategies to cope with aspects of learning that are difficult for them. It is important to recognize these needs early on to minimize frustration and maximize success at school.
Looking ahead
Babies born with spina bifida require ongoing assessment as they grow and develop. They benefit from a multidisciplinary team with expertise in caring for children with spina bifida to optimize their health, functional abilities and independence.
Resources
There are many resources available to help you learn more about spina bifida.
Hydrocephalus Canada
https://www.hydrocephalus.ca/
Spina Bifida and Hydrocephalus Association of Canada
https://sbhac.ca/
Spina Bifida Association
https://www.spinabifidaassociation.org/
Holland Bloorview Kids Rehabilitation Hospital - 'Understanding Spina Bifida' is an excellent resource for parents of children with spina bifida.
https://hollandbloorview.ca/services/programs-services/spina-bifida-and-spinal-cord-services