What is HIV?
HIV stands for Human Immunodeficiency Virus. HIV is a virus that infects certain cells of the immune system. It makes the immune system weaker over time. This puts a person at risk for other serious infections.
A woman who is infected with HIV (HIV-positive) can unknowingly pass the infection onto her baby during pregnancy, at birth or through breastfeeding. Some women do not know they have HIV until they are pregnant and get tested.
Healthy pregnancy and HIV
All pregnant women or women who are considering pregnancy should have a test for HIV. If you are HIV-positive, you should be seeing an HIV specialist. There is no cure for HIV, but there are many medicines that can help keep you healthy. Some medicines are not safe during pregnancy. Your HIV specialist will recommend the safest and best combination of medications for you during your pregnancy.
Your HIV specialist will monitor the amount of HIV in your blood (viral load) to make sure the medicines are working. Keeping your viral load under control will help protect your baby from getting infected with HIV.
You should also see an obstetrician during your pregnancy. An obstetrician is a doctor who has received special training in the care of women during pregnancy, labour and delivery, and the first few weeks after childbirth.
Your family doctor or the clinic where you were diagnosed can refer you to an HIV specialist and an obstetrician.
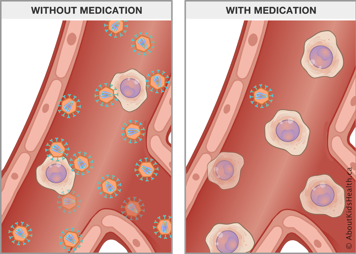
Taking HIV medicine during pregnancy lowers the risk of passing the virus to your baby
If a pregnant woman has HIV and does not receive medicine during pregnancy or delivery, the risk of infection for the baby is around 25%. This means one in four babies will be infected.
The risk that your baby will be infected with HIV is much lower if:
- You take HIV medicines regularly as prescribed.
- Your health-care team knows about your condition so they can deliver proper care during childbirth.
- After being born, your baby takes medicines for six weeks.
- You give formula to your baby and do not breast feed.
In this case, the risk of infection to your baby is less than 1%. This means that fewer than one in 100 babies will be infected.
When and how long you take HIV medicine depends on your situation
Your HIV specialist will discuss the timing of your HIV medicine with you.
- If you need to take medicine for your own health, you will keep taking medicine after your baby is born.
- If you do not need HIV medicine for your own health, you still need to take medication during your pregnancy. When your baby is born, talk to your HIV specialist about your medicine to see if you should continue taking them or not.
Normal delivery vs. C-section (caesarean section)
If your viral load is greater than 1000 copies/mL near the time of delivery, having a C-section will reduce the risk of passing HIV to your baby. A high viral load can happen for any of these reasons:
- if the medicines are not working, that is if the virus is resistant to the combination of medicines you are taking
- if you started taking medicine late in the pregnancy
- if you are not taking the medicine regularly
If your viral load is less than 1000 copies/mL, your obstetrician will not likely recommend you have a C-section. It's easier for you to recover for a vaginal delivery. Also, a C-section will not be safer for your baby.
Talk to your HIV specialist and your obstetrician about what kind of delivery is best for you.
What to do when you go into labour
Keep taking your medicines, even when you start to go into labour. Go to the hospital soon after you suspect you are in labour. You should be given an additional medicine called zidovudine (AZT) intravenously. It is best to receive it at least two to four hours before the baby is born.
What to expect when your baby is born

Do not breastfeed your baby. Give formula instead. Breastfeeding is one way of passing HIV from mother to child.
For more information, please read HIV and your baby.
Your baby will be given AZT within the first 24 hours after birth. You will need to give your baby this medicine twice a day for the first six weeks of life. This can further reduce the risk of HIV infection in your baby. Your baby will also need blood tests for HIV.
For more information
If you are planning on getting pregnant, talk to your health-care provider. They can help you make the safest choices. For more information, please visit https://www.thebodypro.com/article/reproductive-options-hiv-infected-patients
If you have any questions or concerns, contact your doctor or the HIV clinic. For more information, please see the following:
- CATIE: Community AIDS Treatment Information Exchange www.catie.ca
