What is pleural effusion?
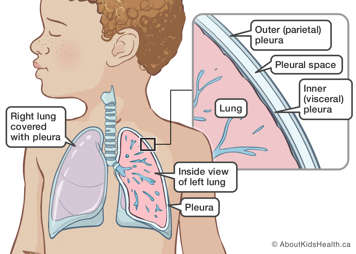
The lungs are surrounded by a membrane called the pleura:
- The parietal pleura is the outside membrane.
- The visceral pleura is the inside membrane, attached to the lungs.
Between the pleural membranes, in the area surrounding the lungs, is the pleural space. Sometimes, there can be a buildup of fluid in the pleural space. This is called a pleural effusion. This buildup of fluid can put pressure on the lungs and make breathing more difficult.
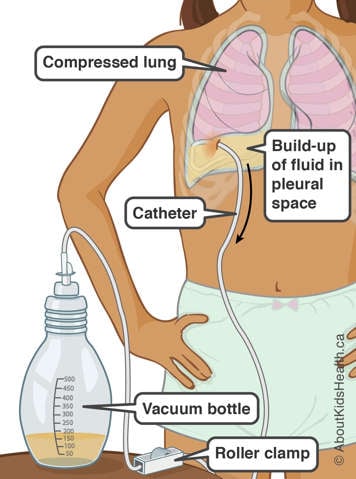
Catheter drainage for pleural effusion
A catheter is a small tube. For a pleural effusion, a catheter is inserted into the pleural space to drain the fluid that is making your child feel short of breath. The goal of inserting the catheter is to allow your child to remain as active as possible, and to improve their quality of life. Your child’s health-care team will teach you how to connect the catheter to a vacuum bottle so that you can drain the fluid from around your child’s lung. They will also provide you with information about ordering equipment, making dressing changes, changing the valve cap, and who to contact if you require more information.
How are drainage catheters inserted?
The drainage catheter is placed by an interventional radiologist in the location that will result in the best fluid drainage. The drainage catheter helps children manage recurrent buildup of fluid in the pleural space at home. The system includes a catheter that is inserted into the body, and vacuum bottles that allow fluid to be drained quickly, effectively and safely.
More than one tube may be placed if there is fluid around both lungs or if there are large, separate pockets of fluid. Local anesthetic will be used (even if your child has been given a general anesthetic and is asleep), as it helps reduce the amount of pain your child will feel after the tube(s) are placed.
A small needle is placed into the fluid around the lungs with the assistance of ultrasound. Two small incisions are then made in the skin, one where the needle goes in and another further down the chest or abdomen where the catheter comes out. The catheter is placed under the skin and into the pleural space. The position of the catheter is then checked with X-rays. Once in the correct place, the catheter is secured with a dressing to protect it. If your child is staying in the hospital, the catheter may be attached to a drainage box or bottle.
Risks of catheter drainage for pleural effusion
A drainage catheter insertion is usually a low-risk procedure. The risk may increase depending on your child’s condition, age and health.
The risks of a drainage catheter insertion can include:
- pain or discomfort
- bleeding
- leakage of air back into the pleural space
- infection
- worsening breathing problems
- X-ray exposure
Preparing for a drainage catheter insertion
Giving consent before the procedure
Before the procedure, the interventional radiologist will go over how and why the procedure is done, as well as the potential benefits and risks. They will also discuss what will be done to reduce these risks and will help you weigh any benefits against them. It is important that you understand all these potential risks and benefits of the drainage catheter insertion and that all your questions are answered. If you agree to the procedure, you can give consent for treatment by signing the consent form. A parent or legal guardian must sign the consent form for young children. The procedure will not be done unless you give your consent.
How to prepare your child for the procedure
Before any treatment, it is important to talk to your child about what will happen. When talking to your child, use words they can understand. Let your child know that medicines will be given to them to make them feel comfortable during the procedure.
Children feel less anxious and scared when they know what to expect. Children also feel less worried when they see their parents are calm and supportive.
Food, drink, and medicines before the procedure
- Your child’s stomach must be empty prior and during sedation or general anesthetic.
- If your child has special needs during fasting, talk to their health-care provider to make a plan.
- Your child can take their regular morning medicine with a sip of water two hours before the procedure.
- Medicines such as acetylsalicylic acid (ASA), naproxen or ibuprofen, warfarin, or enoxaparin may increase the risk of bleeding. Do not give these to your child before the procedure unless they have been cleared first by their health-care provider and the interventional radiologist.
On the day of the drainage catheter insertion for pleural effusion
Your child will have medicine for pain
It is important that your child is as comfortable as possible for the procedure. They may be given local anesthesia, sedation or general anaesthesia. The type of medicine that your child will have for the procedure will depend on your child’s age and condition.
During the catheter insertion, you will be asked to wait in the waiting area.
After the drainage catheter insertion
Once the catheter insertion is complete, your child will be moved to the recovery area. The interventional radiologist will come and talk to you about the details of the procedure. If it was done under sedation or general anesthesia, as soon as your child starts to wake up, a nurse will come get you.
Some children feel local pain or discomfort after the catheter is placed. Your child will be closely monitored and given pain medicine as needed. After a day, most children feel no pain with the catheter.
After the procedure, the tube will be connected to a drainage collection system if your child has a large pleural effusion, or the tube may be closed with a valve cap if enough fluid was removed during the procedure. Your child’s health-care team will teach you how to connect the catheter to the vacuum bottles so that you can drain the fluid from around your child’s lung every day (or as directed by your child’s health-care team).
Potential drainage catheter complications at home
No drainage
If fluid stops draining, it could be because:
- there is no fluid left in the pleural space
- the catheter or system drainage line is blocked
It is uncommon for either the catheter or the system drainage line to become blocked. If you think the catheter or drainage line may be blocked, squeeze them gently. If drainage does not start again, follow the instructions that came with your drainage system for how to change to another bottle. If drainage does not start when you switch to a second bottle, call your child's health-care team. They may order a test (such as an ultrasound or CT scan) to determine how much fluid is in the pleural space, if medication is needed to unblock the catheter, or if the catheter needs to be changed or removed.
Site issues
- Some discomfort and mild redness are expected after insertion but should not worsen or last longer than one week.
- If the catheter is pulled out, or the catheter cuff becomes exposed, cover the exit site with a sterile self-adhesive dressing and seek immediate medical attention.
- If your child’s dressing is wet or loose, change it using the sterile technique you have been taught by their health-care team.
Damaged, cut or broken catheter
Pinch the catheter closed between your fingers if the catheter becomes damaged, cut or broken. If you have a slide clamp provided in your drainage system kit, slip it over the catheter and tighten the clamp. If you do not have a slide clamp, bend the catheter and tape it in this position. Call your child’s health-care provider immediately.
Disconnected valve or valve malfunction
If there are problems with the catheter valve, get a new valve cap and wipe it with an alcohol pad. Place it over the catheter valve and twist it clockwise until it clicks and locks. A damaged valve may allow air into your child's body or let fluid leak out through the valve.
When to seek medical assistance
After the catheter has been inserted and you are home, you should call your child's health-care team, or go to the nearest Emergency Department if your child develops any of the following:
- Your child has a fever measured orally:
- temperature is 38.3°C or more by mouth one time, or;
- temperature is 38°C or more by mouth for one hour or more.
- Your child has a fever measured under their arm:
- temperature is 37.8°C or more under the arm one time, or;
- temperature is 37.5°C or more under the arm for one hour or more.
- temperature is 37.8°C or more under the arm one time, or;
- There is a change in the colour, consistency or amount of fluid draining from your child’s chest.
- Your child has pain when you are draining fluid from their chest or pain that continues after draining.
- Your child has redness, swelling, drainage or pain at the catheter insertion site or in the region of the catheter.
- You damage, break or cut the catheter, or it becomes dislodged.
- You see fluid leaking from the valve or catheter.
At SickKids
If you have any concerns related to your child’s drainage catheter, please ask your home visiting nurses first; or contact your child’s Oncology clinic nurse during working hours. If you have concerns and it is after working hours, call The Hospital for Sick Children switchboard at (416) 813-7500 and ask them to page the Oncology fellow on call.
Resources
SickKids uses a brand of drainage catheters called PleurX drainage systems. For more information on the PleurX drainage system, visit the PleurX drainage system website.
PleurX resources
Watch a video on how to drain pleural effusions at home: PleurX® with roller clamp patient education.
How to Drain Using the PleurX Lockable Drainage line Kit.pdf