What is facioscapulohumeral muscular dystrophy?
Facioscapulohumeral muscular dystrophy (FSHD) is a genetic condition that causes progressive weakness and loss of muscle bulk (atrophy) of skeletal muscles. It most commonly affects the muscles of the face (facio-), shoulder blades (scapulo-) and upper arms (humeral), though it can later involve muscles in the lower body.
The disease is linked to abnormal expression of the DUX4 gene on chromosome 4. Normally, this gene is turned off before birth, but in FSHD, changes in the region of the chromosome containing the DUX4 gene cause it to be turned on. This leads to the production of the DUX4 protein in muscle cells, where it damages the muscle cells. Over time, the muscle cells die and are replaced with fat and fibrous tissue.
FSHD is one of the more common muscular dystrophies, affecting both children and adults. It is seen in about 1 in 14,000 people. The most common form is known as FSHD type 1, which is linked to changes on chromosome 4.
Most people with FSHD will start showing symptoms before age 20. However, FSHD can be very variable in its severity. Up to about one-third of gene carriers may have very mild symptoms or, in some cases, may not show any noticeable symptoms at all.
Signs and symptoms of FSHD
- Facial weakness: Difficulty making facial expressions due to muscle weakness.
- Winged scapula (shoulder blade): The shoulder blade sticks out, making day-to-day activities, such as lifting grocery bags or brushing teeth, difficult.
- Muscle weakness: Progressive weakness typically begins in the upper body and may extend to the trunk and legs.
- Upper arm muscle weakness
- Abdominal muscle weakness, leading to lordosis (inward curve of the spine)
- Pelvic weakness in adulthood
- Foot drop
- Fatigue and pain
FSHD can sometimes cause non-muscular symptoms such as:
- Hearing loss, specifically high frequencies (high pitches)
- Retinal changes in the eyes
- Heart problems such as atrial arrhythmias
- Breathing difficulties
- Intellectual disability
- Seizures
Cause of FSHD
FSHD is an inherited condition, meaning it is passed from parents to their children through genes. Genes are the instructions that our cells use to make proteins. They tell our cells how to work and what to do. Each person carries two copies of each gene. A child gets (inherits) one copy from their mother and the other from their father.
FSHD is a genetic disease caused by changes in a gene called DUX4. This gene is located in an area called the D4Z4 region of chromosome 4. The D4Z4 region is normally repeated 11 to more than 100 times, and each repeated section contains a DUX4 gene. When there is a large number of repeats, the DUX4 gene is turned off before birth. People with FSHD have fewer D4Z4 repeats, between 1 and 10. Having fewer repeats causes the DUX4 gene to become active again in muscle cells, which damages muscle cells, causing them to die and be replaced by fat.
FSHD can affect a child in two ways: either through inheritance from a parent who has the condition or through a new, spontaneous change in the child’s genes, known as a de novo mutation.
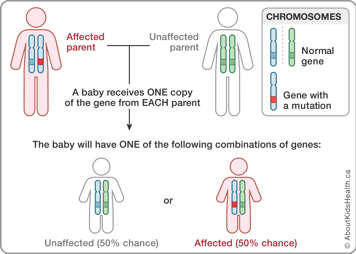
When it is inherited from a parent it is in an autosomal dominant pattern. Autosomal dominant inheritance occurs when one parent is affected with the disorder and the other parent is unaffected. One normal gene from the unaffected parent and one gene with a mutation from the affected parent are passed down to the child. In autosomal dominant inheritance, only one abnormal copy of the gene is needed to cause disease. A parent affected with the disorder has a 50% chance of passing the condition on to the child.
If your child is confirmed to have FSHD, meeting with a geneticist or physician when they grow up can be very helpful. They can provide guidance and information about family planning in the future, which can help them and their potential partner make informed decisions.
Course and progression of FSHD
The severity of FSHD and how fast it progresses can be very variable. The progression in children can be rapid, especially in those with very few D4Z4 repeats (1 to 3 repeats), leading to a more severe disease. Children with very few repeats (1 to 3 repeats) tend to have a more severe disease course. Moreover, early-onset FSHD is associated with additional symptoms such as hearing loss, retinal problems, central nervous system involvement and difficulties with eating or breathing. These symptoms are more common in children with very few D4Z4 repeats.
How is FSHD diagnosed?
FSHD is diagnosed through genetic testing via a blood test.
Treatment of FSHD
There is currently no cure for FSHD, treatment is focused on a multidisciplinary approach to supportive care. Follow-up care is essential for children with FSHD. Regular visits with the multidisciplinary team help them to stay on top of any changes in the condition and adjust treatment as needed to support your child’s health.
Your child’s health-care team may include:
- Neurologist: Diagnoses and monitors FSHD, managing symptoms such as muscle weakness and fatigue.
- Physical therapist: Develops exercise plans to maintain strength and flexibility.
- Occupational therapist: Helps with daily tasks and manages fatigue and pain.
- Orthopedic surgeon: Treats joint and bone issues and may recommend supportive devices.
- Speech therapist: Assists with speech and swallowing difficulties caused by facial weakness.
- Psychologist or counsellor: Provides emotional support and coping strategies.
- Genetic counsellor: Explains the genetic aspects of FSHD and its inheritance patterns.
- Audiologist and ophthalmologist: Monitors for rare hearing and vision issues.
- Cardiologist: Keeps an eye on heart health, though issues are uncommon in FSHD.
This multidisciplinary care approach addresses both the physical and emotional aspects of FSHD, helping to improve the child's quality of life.
Genetic counselling
Genetic counselling can be a valuable resource for families. A genetic counsellor can provide support by explaining test results and helping families understand the implications of a FSHD diagnosis. They can also discuss prenatal testing options if there is a family history of FSHD or if a family member has tested positive for a FSHD-related mutation. Genetic counselling can be especially useful in planning for future family decisions and managing the impact of FSHD on family life.
How can I help at home?
Caring for your child at home and adapting to their unique needs is at the heart of managing their condition. Keeping up with physical therapy, doing strengthening exercises and following lifestyle tips from different therapists are essential because home care is just as important as hospital care. Psychological counselling or support groups can also be very helpful, not only for children with FSHD but for their families as well.
At SickKids
SickKids has a specialized neuromuscular clinic that focuses on FSHD and similar conditions. Located within the neurology department, the clinic is staffed by a neurologist, nurse practitioner, and experienced technicians who are dedicated to caring for children with FSHD. Our clinic visits range from simple follow-ups to more specialized procedures, such as nerve conduction studies and electromyography. Additionally, we offer access to a professional social worker who can provide support for both you and your child and connect you with relevant support groups if needed. You are not alone in this journey!
https://www.sickkids.ca/en/care-services/clinical-departments/neurology/neuromuscular-program/
Resources
FSHD Canada Foundation
fshd.ca
FSHD Society
fshdsociety.org
Facioscapulohumeral Muscular Dystrophy (FSH, FSHD) - Muscular Dystrophy Association
mda.org/disease/facioscapulohumeral-muscular-dystrophy
Facioscapulohumeral Dystrophy - Medscape
emedicine.medscape.com/article/1176126-overview?form=fpf#a5
ClinicalTrials.gov
clinicaltrials.gov
Facioscapulohumeral muscular dystrophy (FSHD) - Muscular Dystrophy UK
musculardystrophyuk.org/conditions/a-z/facioscapulohumeral-muscular-dystrophy-fshd/
References
FSHD Canada Foundation. Incidence of FSHD. https://fshd.ca/overview/incidence-of-fshd/
Chen, T.H., Wu, Y.Z., & Tseng, Y.H. (2020). Early-Onset Infantile Facioscapulohumeral Muscular Dystrophy: A Timely Review. International Journal of Molecular Sciences, 21(20), 7783. https://doi.org/10.3390/ijms21207783
Goselink R.J.M., Schreuder, T.H.A., van Alfen, N., de Groot, I.J.M., Jansen, M., Lemmers R.J.L.F., van der Vliet, P.J., van der Stoep, N., Theelen, T., Voermans, N.C., van der Maarel, S.M., van Engelen, B.G.M., & Erasmus, C.E. (2018). Facioscapulohumeral Dystrophy in Childhood: A Nationwide Natural History Study. Annals of Neurology, 84(5), 627-637. https://doi.org/10.1002/ana.25326