What is myotonic dystrophy type 1?
Myotonic dystrophy type 1 (DM1) is a genetic disorder characterized by progressive muscle weakness and myotonia (inability of the muscles to relax after contraction). It is caused by a mutation in the DMPK gene and is inherited in an autosomal dominant manner, meaning only one copy of the mutated gene is needed to cause the disorder. Symptoms can include muscle wasting, cataracts, cardiac issues and endocrine disturbances.
What are the signs and symptoms of DM1?
DM1 can cause many different symptoms, and they may vary a lot from one person to another. Common signs and symptoms include:
- Muscle weakness and shrinking: Muscles can slowly become weaker and get smaller. This is often seen in the face, neck and lower legs.
- Muscle stiffness (myotonia): After moving or using muscles, they may take a long time to relax, which can feel like stiffness.
- Cataracts: The lens in the eye can become cloudy, making it hard to see clearly.
- Heart problems: The heart’s electrical system might not work normally, which can cause an irregular heartbeat or other heart issues.
- Breathing difficulties: Muscles that help you breathe may be weak and can make it hard to breathe, especially when you are sleeping.
- Digestive problems: The muscles that help move food through the body may not work well, leading to trouble swallowing, constipation, or other stomach problems.
- Hormone problems: Some people may have issues such as insulin resistance (which can lead to diabetes), thyroid problems or low testosterone in men.
- Tiredness and sleepiness: Many people feel very tired during the day and may have a hard time staying awake.
- Learning and mood challenges: Some people might have trouble with learning, memory or concentration and they might also have mood swings.
- Speech and swallowing issues: It can become difficult to speak clearly or swallow food and drinks.
Differences between congenital and later-onset DM1
Congenital myotonic dystrophy (present at birth)
Babies with congenital DM1 often show signs of muscle weakness right from birth. They may have trouble feeding and breathing properly. The health challenges for babies with congenital DM1 are usually more serious. They might need special care right away after birth and throughout their childhood. Because the symptoms are severe from the start, the long-term outlook is more uncertain. Children often face major challenges as they grow, including significant muscle weakness, learning problems and other health issues. Early intervention and ongoing care are very important.
Later-onset myotonic dystrophy (teenagers or adults)
People with later-onset DM1 usually start to show symptoms later in life, such as in their teenage years or adulthood. The symptoms, such as muscle weakness and stiffness, tend to develop more slowly at first. Although they have similar types of problems as those with the congenital form, the issues are generally less severe in the beginning. However, over time, these symptoms can worsen.
What causes DM1
DM1 is a genetic disorder that happens because of a mutation in the DMPK gene on chromosome 19. The mutation causes a segment of the DNA to be repeated too many times. This extra-long section of DNA disrupts the production and control of important proteins in the body. As the number of these repeats increases, so does the severity of the symptoms. The number of repeats can grow larger with each generation, causing children to develop symptoms earlier and/or more severely than their parents. Although DM1 is relatively rare, it affects about one in every 8,000 people.
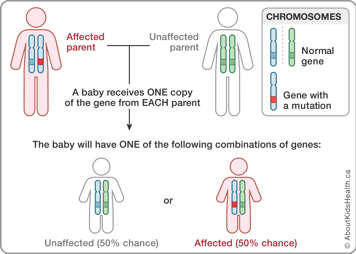
The disorder is usually passed down in an autosomal dominant pattern. Autosomal dominant inheritance occurs when one parent is affected with the disorder, and the other parent is unaffected. One normal gene from the unaffected parent, and one gene with a mutation from the affected parent, are passed down to the child. In autosomal dominant inheritance, only one abnormal copy of the gene is needed to cause disease. A parent affected with the disorder has a 50% chance of passing the condition on to the child.
How is DM1 diagnosed?
- Clinical examination: The health-care team will look for signs such as weak muscles and muscles that take a long time to relax.
- Genetic testing: A small amount of blood is taken to study the DMPK gene to see if there are extra repeats in the gene, which are the cause of DM1. This test confirms whether the gene mutation is present.
- Electromyography (EMG): EMG uses small needles to measure the electrical signals in the muscles. This test shows how well the muscles work and helps confirm if the muscle problems are due to DM1.
How is DM1 treated?
There is currently no cure for DM1, but several treatments can help manage symptoms and improve quality of life. The main goal of treatment is to help children stay active and maintain independence. A multidisciplinary approach is crucial to improving the quality of life for people with DM1.
Treatments include:
- Symptom management:
- Muscle weakness and myotonia: Medications such as mexiletine can help reduce myotonia. Physical therapy and regular exercise can improve muscle strength and flexibility.
- Cardiac care:
- Regular cardiac evaluations, including ECG and echocardiograms, are essential.
- Medications to manage arrhythmias or other heart conditions, and in some cases, the use of pacemakers or implantable cardioverter-defibrillators (ICDs).
- Respiratory support:
- Regular monitoring of respiratory function.
- Non-invasive ventilation support, such as continuous positive airway pressure (CPAP) or bilevel positive airway pressure (BiPAP) for those with sleep apnea or respiratory insufficiency.
- Supplemental oxygen or, in severe cases, mechanical ventilation.
- Gastrointestinal and nutritional support:
- Dietary modifications and nutritional support to manage dysphagia and gastrointestinal motility issues.
- Speech therapy to help with swallowing difficulties.
- Endocrine and metabolic management:
- Regular screening and management of diabetes, thyroid dysfunction and other endocrine abnormalities.
- Insulin or other medications to manage diabetes.
- Ophthalmologic care:
- Regular eye examinations to monitor and treat cataracts, which may require surgical intervention.
- Psychological and cognitive support:
- Cognitive behavioral therapy and other psychological support for managing depression, anxiety and other mental health issues.
- Educational support and strategies to address cognitive impairments.
- Genetic counselling:
- Genetic counselling for affected individuals and their families to discuss inheritance patterns, family planning and potential risks to future generations.
- Supportive therapies:
- Occupational therapy to help with daily living activities and to recommend assistive devices if needed.
- Social support and engagement with patient support groups and resources for additional help and community connection.
- Regular monitoring and multidisciplinary care:
- Regular follow-ups with a multidisciplinary team, including neurologists, cardiologists, pulmonologists, endocrinologists and other specialists, to monitor and manage the various aspects of the disease.
- Muscle weakness and wasting: Progressive muscle weakness and atrophy, particularly in the face, neck and distal limbs, can lead to difficulties in mobility and daily activities.
- Cardiac issues: Arrhythmias, conduction defects and cardiomyopathy, which can lead to heart failure or sudden cardiac death.
- Respiratory complications: Weakness of respiratory muscles, leading to respiratory insufficiency, hypoventilation and increased risk of pneumonia.
- Cataracts: Early-onset cataracts, often developing in childhood or early adulthood can affect vision
- Endocrine abnormalities: Insulin resistance, diabetes, thyroid dysfunction and issues with reproductive hormones.
- Cognitive and behavioral issues: Learning disabilities, cognitive impairment and in some cases, psychiatric disorders such as depression and anxiety.
- Gastrointestinal problems: Dysphagia (difficulty swallowing), constipation and other gastrointestinal motility issues can affect nutrition and growth
- Sleep disorders: Excessive daytime sleepiness, sleep apnea and other sleep-related breathing disorders.
- Fertility and pregnancy issues: In men, testicular atrophy and infertility. In women, complications during pregnancy, such as preterm labor and delivery.
- Pain: Chronic pain due to muscle cramps, stiffness and joint issues.
- Hypersomnia: Excessive daytime sleepiness not related to sleep apnea, making it difficult to stay awake during the day.
Genetic counselling
Genetic counselling can be a valuable resource for families coping with the challenges of DM1. A genetic counsellor can provide support by explaining test results and helping families understand the implications of a DM1 diagnosis. They can also discuss prenatal testing options if there is a family history of DM1 or if a family member has tested positive for a DM1-related mutation. Genetic counselling can be especially useful in planning for future family decisions and managing the impact of DM1 on family life.
Support
Connecting with others who have experience with DM1 can provide a strong support network for families. Psychological counselling or participation in support groups can be beneficial both before and after a diagnosis, offering emotional support for children with DM1 and their families. These resources help families navigate the challenges of DM1 and provide a space for shared experiences and guidance.
At SickKids
SickKids has a specialized neuromuscular clinic that focuses on DM1 and similar conditions. Located within the neurology department, the clinic is staffed by a neurologist, nurse practitioner and experienced technicians who are dedicated to caring for children with DM1. Our clinic visits range from simple follow-ups to more specialized procedures, such as nerve conduction studies and electromyography. Additionally, we offer access to a professional social worker who can provide support for both you and your child and connect you with relevant support groups if needed. You are not alone in this journey!
https://www.sickkids.ca/en/care-services/clinical-departments/neurology/neuromuscular-program/
Resources
Myotonic Dystrophy Foundation (MDF)
myotonic.org
National Institute of Neurological Disorders and Stroke (NINDS) - USA
ninds.nih.gov
The Genetic and Rare Diseases (GARD) Information Center
rarediseases.info.nih.gov
Rare Diseases International (RDI)
rarediseasesinternational.org
Orphanet
orpha.net
World Muscle Society (WMS)
worldmusclesociety.org
References
Rahm, L., Hale, M.A., Raaijmakers, R.H.L, Marrero Quiñones, A., Patki, T., Johnson, N.E., van Bokhoven, H., & Karlien, M. (2025). Myotonic dystrophy type 1: clinical diversity, molecular insights and therapeutic perspectives. Nature Reviews Neurology, 21, 623 641. https://doi.org/10.1038/s41582-025-01139-x
Johnson N.E., Aldana E.Z., Angeard N., Ashizawa T., Berggren K.N., Marini-Bettolo C., Duong T., Ekström A.B., Sansone V., Tian C., Hellerstein L., & Campbell C. (2019). Consensus-based care recommendations for congenital and childhood-onset myotonic dystrophy type 1. Neurology Clinical Practice, 9(5), 443-454. https://doi.org/10.1212/CPJ.0000000000000646
Ho, G., Cardamone, M., & Farrar, M. (2015). Congenital and childhood myotonic dystrophy: Current aspects of disease and future directions. World Journal of Clinical Pediatrics, 4(4), 66-80. https://doi.org/10.5409/wjcp.v4.i4.66
Campbell, C., Levin, S., Siu, V.M., Venance, S., & Jacob, P. (2013). Congenital myotonic dystrophy: Canadian population-based surveillance study. The Journal of Pediatrics, 163, 120-123. https://doi.org/10.1016/j.jpeds.2012.12.070